Thinking About Suicide? Here’s How to Get the Right Help
Going through a mental health crisis can be one of the loneliest experiences you’ll ever have.
Some people call it “the dark night of the soul.” Others call it “rock bottom.” Whatever you call it, despair is heavy and hard to navigate. When psychological pain, trauma, social isolation, or personal hardship bring you to a point that you’re thinking about suicide, it can feel impossible to move past it.
HEADS UP
If You're In Crisis, Get the Right Care Right Away
If you’ve had more than vague, passing thoughts about suicide, you may need more than therapy.
If you’ve been thinking about suicide a lot, feeling like you want to die instead of vaguely wondering if you’d be “better off dead,” or planning how you might end your life, you’re at an elevated risk of suicide and should call the National Suicide Prevention Lifeline, a local crisis line, 911, or an international crisis line.
No matter where you call, the person who answers will talk to you about what you’re going through and help you get the right level of care.
Instinct drives us to ask for help when we become lost, but hopelessness defies that instinct. But even when you do reach out, many people don’t know what to say or how to help when you tell them you’re not sure you can go on living. They might panic, stumble over their words, minimize your pain, or give you a few awkward platitudes. You might even have been turned away by a therapist.
When your first attempt to ask for help fails, it’s easy to shut down and fall further into the vortex of suicidal thoughts. It can seem like the world is confirming what your renegade brain keeps telling you: that you’re not worthy of help or that you can’t be helped. It might feel like no one can reach you where you are and that it’s impossible to climb out on your own.
But it's not true. There is help, and with it, you can recover a sense of space and possibility. You can get through the long, dark hallway—it isn't endless, after all—and emerge from that claustrophobic place.
Suicidal despair can actually be a turning point, the first light of clarity after a long night of confusion: the point you know you need to address the internal or external issues that brought you to this place. All you need to do to step out of the darkness and into the light is to know who to talk to and what to tell them to get the help you need.
On This Page
You Can Get Help Even If You Haven't Found It Yet
One of the first steps in finding your way out of the dark hall of despair is understanding that two things are true:
- Few people understand how to help someone who’s thinking of suicide; but
- Some people do.
It’s important to know that you are not alone. You are not alone in having reached this place; other people have been here and have found a way out. You are not alone in navigating your way out of it, either; there are people who aren’t afraid to look into the abyss with you and who can help you cross it.
If loved ones have made you feel like you shouldn’t talk about what you’re thinking or feeling, they’re wrong. It can help to understand that they’re probably afraid. They probably want to help you, but they don’t know how.
If a therapist turned you away, understand that there are specific reasons that this happened, none of which mean you can’t get the help you need. It just means that right now, you probably need a higher level of care than individual therapy sessions.
If you don't specify what kind of suicidal thoughts you're having, most therapists default out of caution to thinking you've reached a level of crisis they can't address.
There are different levels of risk associated with different types of suicidal thoughts. You may well have reached a crisis point that requires inpatient care, or you might be a perfect candidate for therapy. You can find out which is true by learning what your risk level is.
Before we review this information, though, it’s important to understand that it’s not your job to figure out your suicide risk level. If reading this is difficult for you and you just want to talk to someone, that is a wise and valid response to your circumstances.
There are many places you can (and should) call for help (see the information box immediately below). The people who answer will listen with compassion and can help connect you with local mental health treatment options.
Where to Call for Help
If you’re going through a mental health crisis, there’s someone you can call.
If you’re at immediate risk of harm, or have already harmed yourself, you should call 911 immediately.
If you’re thinking of suicide, but are not at immediate risk of harm if you don’t get medical intervention right away, you should call the National Suicide Prevention Lifeline at 988 or a local mental health crisis hotline.
For lists of different mental health crisis hotlines you can call, you can go to any of the following pages on our site:
- National and International Suicide Hotlines
- Free Mental Health Hotlines in the United States
- The United States Mental Health Services Guide
On that last page, you can find information specific to your state, including the mental health crisis hotline for your city or county. Just select your state to get the local information you need.
Assessing Suicide Risk
The first time you think about suicide, you’re more likely to think about it vaguely, in response to pain or hopelessness. For example, you might think, “Maybe I’d be better off dead.”
If you’re like many people, you’ve had such a thought, immediately followed by all the reasons you want to be alive and the reasons you wouldn’t end your own life. Just because you’ve ever had a thought like that doesn’t mean you’re in crisis now or need emergency care.
Your suicide risk level is higher if you've thought about suicide recently. It increases as you think about suicide more often and in greater detail.
More than therapy is needed when suicidal thoughts develop two dangerous features: intent and a plan. If you’ve progressed from considering suicide to actively wanting to end your life, you’re in much greater danger than when the thoughts are vague or passive.
Your risk of acting on the thoughts is even higher if you’ve started planning how you would end your life. Using substances also increases your suicide risk by increasing your risk of acting on a sudden impulse.
The following infographic shows the risk levels associated with each kind of suicidal thinking and the recommended level of care for each:
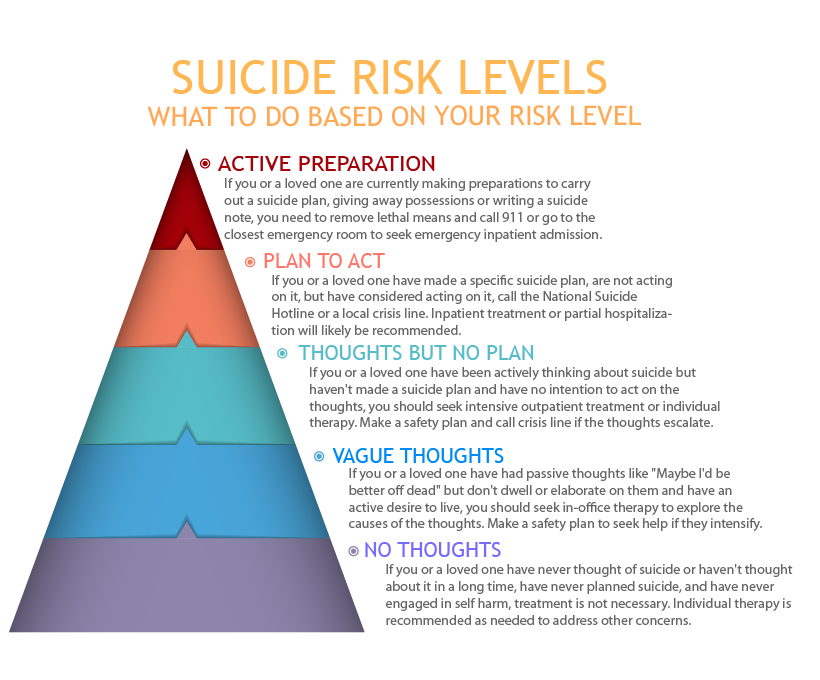
When you’re actively considering suicide, you’re in crisis and need something more intensive than a weekly therapy session. When you’ve reached the point you’re planning to act, you need to immediately seek emergency care. If you’re not sure where to go, please call 988 or one of the other numbers listed above to connect with the care you need.
Risk and Protective Factors
When mental health professionals evaluate your suicide risk, they also consider what they call risk and protective factors. These are aspects of your life that either increase or lower your risk of suicide.
Knowing which of these you have—and how many—can help professionals (and you) figure out what level of support and care you need right now. In general, the fewer protective factors you have, the higher level of care you need.
You’re more at risk of acting on thoughts of suicide if you’re struggling with pain, trauma, or chronic stress at work or home and aren’t talking to anyone about it.
You’re less likely to act on suicidal thoughts when you feel supported and connected, whether it’s to a therapist, friends, family, or a community of like-minded individuals.
One of the important things to understand about depression is that it isolates you and convinces you that you’re alone because you deserve to be or because there’s something wrong with you. This isn’t true. Many more people than you’d think go through periods of isolation; they just don’t tell people how lonely it got for them.
Just like thoughts of suicide can be overcome, so can social isolation. The more connected the world becomes, the more we all learn we have a tribe out there somewhere. You can find yours and enjoy a very different quality of life than what feels possible for you now. Getting the help you need to get through a crisis is often only the first step on the journey of healing.
Getting the Right Level of Care for Your Risk Level
Therapists who work online are often more reluctant to provide care to clients who report suicidal thoughts even when therapy is the right level of care.
This may have less to do with concerns about the limitations of online therapy than it does with how much harder it is to accurately screen for suicide risk using an online form. Many times, if you select the “wrong” box, you’re automatically routed somewhere else—like this page—without the chance to explain further.
It also has to do with the importance of in-person supports for people with severe symptoms. While online therapy can be as effective as in-office therapy, there are times when it isn’t. It’s much easier for your therapist to help you create and follow a safety plan and link you with other local resources when they’re part of your local community and you see them in person.
PRO TIP
While it’s not necessary or your job to figure out your suicide risk level, knowing it, or at least knowing what kinds of thoughts you’re having, can help you feel more confident when you talk to mental health professionals and can help you collaborate with them to get the right level of care.
To get the right care for your risk level, your best option is to connect with someone local—whether it’s a local therapist or a local mental health hotline. The National Suicide Prevention Lifeline (988) is also a good place to call. It’s staffed with people who understand suicidal thoughts and feelings and address them with nuance and respect.
How to Get the Care You Need
Two ways to get mental health care immediately are to call 911 or go to a local emergency room. If you aren’t in immediate danger if you don’t get medical care right away, and you want to talk to a counselor first, you can call the National Suicide Prevention Lifeline (988) or a local crisis line.
Mental health crisis lines are part of the public mental health system in every state and typically operate 24/7 or have after-hours alternatives. There are also international crisis lines.
DEEP DIVE
For more information on the public mental health system in the United States, including general information on how it works and who it’s for, you can read our article, “The United States Public Mental Health System.”
For more information on your state’s system, including where to call when you’re in crisis, you can go to our United States Mental Health Services Guide and select your state to learn more.
The people who answer crisis and suicide hotlines can give you immediate support and connect you with the care you need. If you need help right away and can’t transport yourself to an emergency room, they may be able to connect you to a local dispatcher and get first responders to come to you.
Note that once first responders become involved, you are no longer in control of all decisions about your care. If you say you’re thinking of harming yourself, then try to leave, you may be temporarily detained for involuntary treatment.
If you’ve had vague or passive suicidal thoughts, no suicide plans, and no intent to act on them, therapy can be a great place to start, especially if you have other protective factors that can help.
PRO TIP
The best way to help a potential therapist accurately assess the care you need is to explain all of your symptoms and circumstances in detail and provide the necessary context to help them determine your risk level. You’ll be able to communicate with more nuance when you’re in the room together.
What to Expect from Therapy
If you and a therapist determine that therapy is appropriate for your risk level, addressing suicidal thoughts will be an important element of your therapy plan, though probably not the only one.
Your therapist will want to explore your personal and mental health history, determine whether you have a mental health condition, and assess your current stressors.
Your therapist will want to understand the factors in your life that affect your mental health the most, whether those are circumstances at work or home or something else. They’ll want to learn more about the specific nature of the thoughts you’re having and develop a safety plan so you’ll know what to do if the thoughts become more intense, frequent, or specific.
As you and your therapist get to know one another better, you’ll start delving deeper and finding out what triggers your suicidal thoughts and other symptoms. You’ll work together to address these triggers and any underlying issues you may have, such as unresolved trauma, untreated depression, or unhealthy life circumstances. You’ll collaborate on an action plan for things to work on in therapy and things to do at home to improve your mental health.
What to Expect from Intermediate Levels of Care
You’ll engage in similar tasks in any mental health program. Higher levels of care usually include individual therapy as part of your treatment plan. Intensive and day programs work not by providing a totally different type of care, but by complementing therapy with additional interventions.
In general, higher levels of care involve spending more time each week in treatment than you would if you were seeing a therapist once a week. Intensive outpatient programs usually provide 6-8 hours of care per week, while partial hospitalization or day treatment programs meet for 8 hours a day, five days a week. Some programs offer flexible scheduling options when those are appropriate for your risk level.
DEEP DIVE
For more information on the different levels of mental health care, including intermediate levels of care like partial hospitalization and intensive outpatient treatment, you can read our article, “Choosing the Right Level of Mental Health Care.”
In partial hospitalization and intensive outpatient programs, you usually participate in individual therapy sessions at least once weekly and sometimes as often as every day. You go to multiple group therapy sessions each week as well as instructional classes where you learn more about your condition or symptoms.
Many intermediate programs offer self-help groups where you can talk to peers without a counselor present. Depending on the program, you may also be able to participate in additional activities or therapies like art therapy or yoga.
What to Expect from Inpatient Care
Inpatient treatment usually involves a similar treatment schedule as partial hospitalization or day treatment programs.
The extra time you spend on an inpatient unit isn’t as much about spending more time in groups or therapy sessions as it is about having extra security and immediate care when you need it. Staff are available around the clock. If you’re in an inpatient program and wake up in the middle of the night in crisis, you can immediately connect with professional care.
DEEP DIVE
For more information on inpatient mental health care, including where you go to get it and what to expect when you’re there, you can read our article, “How Inpatient Mental Health Treatment Works.”
Another important feature of inpatient treatment is that it removes you from circumstances that may be triggering or aggravating suicidal thoughts or other mental health symptoms. This allows you to stabilize in a safe environment and gain perspective on what you need to change at home to improve your mental health.
One of the most important things you’ll do in an inpatient program is work with your care team to develop a discharge plan to make your transition back to life at home smoother. Most people follow up inpatient care with outpatient care.
What Causes Suicidal Thoughts?
Philosopher Friedrich Nietzsche famously said, “The thought of suicide is a great consolation; by means of it, one successfully gets through many bad nights.”
Like musicians who have explored suicide in their song lyrics, Nietzsche didn’t believe people should end their own lives. Instead, he wanted to help people find the strength to rebel against suicidal thoughts and the circumstances that produce them. Like other existentialist philosophers, he believed the only way to overcome suicidal despair was to honestly confront its reality.
Why do people have suicidal thoughts? The main reason people think about suicide is that they want to get out of an unbearable situation or end the pain they’re in. This is why Nietzsche said the thought of suicide can be a consolation—it is preferable to the thought of endless pain or torment.
The problem is that suicide is permanent, while the circumstances that make you think about suicide are not.
Many people who have been in despair and gotten help have later found great happiness that seemed impossible at the time.
Conclusion
Though many people have thought about suicide at some point in their lives, it remains a taboo topic.
Even some mental health professionals are uncomfortable with the topic of suicide and refuse to meet with people who tell them over the phone that they’ve thought about suicide.
If this has happened to you, don’t lose hope. Sometimes, they’re right to refer people to a higher level of care, but sometimes they’re wrong. Sometimes they’re just not experienced enough to know what to do, and default to assuming you need a higher level of care.
Understanding that there are different kinds of suicidal thoughts, being able to identify which kind you’re having, and knowing your risk level can help you work with professionals to get the right level of care.
There are experienced therapists who can help you if you’re not in acute crisis (if you are, please call one of the hotlines listed above), and you’re more likely to get in to see one if you can explain your symptoms in detail. You may have more luck with group practices or community mental health agencies.
You can find both kinds of therapy providers using the search tools on OpenCounseling.com.
No matter what it feels or looks like now, there is hope. You’ve been through a lot, and you’re stronger than you know. Your life has potential that’s hard to see in the dark, so please don’t give up. There are people who care and want to help. The more of them you get to know, and the more you learn about yourself, the closer you’ll be to finding your way out of the darkness.
Related Posts
Stephanie Hairston
Stephanie Hairston is a freelance mental health writer who spent several years in the field of adult mental health before transitioning to professional writing and editing. As a clinical social worker, she provided group and individual therapy, crisis intervention services, and psychological assessments.